Is there an ideal measure of gut health, the way that 20/20 reflects “perfect vision”? Alas, not yet. The science of gut health is quite new, and we are just starting to learn about the complex and myriad interactions between our gastrointestinal (GI) system and its trillions of microbial inhabitants, collectively known as the gut microbiome or gut microbiota.
I’ve read a lot of the scientific studies and have drawn some of my own conclusions, based on my personal experience. Here are 5 principles and tips I use in my daily life. These are in order of increasing difficulty (ie 5 is harder than 1).
These are not all you have to do to be healthy, of course, but our gut is a good place to start!
1. Eat at least 30 different plant foods weekly.
Nature loves diversity. Just look at any natural ecosystem (oceans, rainforests, galaxies) and you’ll find a large number of diverse creatures there, filling every niche and using the resources available in cooperative and symbiotic ways. Well, the same holds true for our gut ecosystem.
Why is a more diverse gut microbiome healthier than one with a few dominant species of microbes? We are still trying to figure out causality, but there are strong associations. We do know that the reduction in intestinal microbiota diversity is associated with human diseases, such as Crohn’s disease, obesity, type 2 diabetes, etc.
Conversely, increased microbial diversity in our gut is associated with higher states of health. According to data collected by the American Gut Project, the number of plant types in a person’s diet plays a role in the diversity of his or her gut microbiome — the number of different types of bacteria living there. No matter the diet they prescribed to (vegetarian, vegan, etc.), participants who ate more than 30 different plant types per week (41 people) had gut microbiomes that were more diverse than those who ate 10 or fewer types of plants per week (44 people). The gut samples of these two groups also differed in the types of molecules present. [source]
Here’s a list of plants I’ve eaten in the past week. I stopped when I reached 30 (there are probably more).
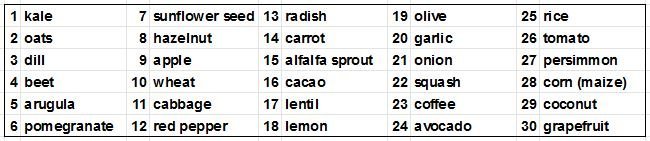
How many plant foods have you eaten lately? Let us know in a comment below!
I’ve also had my gut sampled from the fine folks at the American Gut Project. It’s simple and fun to get your gut sampled and see how your gut critters compare to other people’s!
Do I know exactly how to interpret the results? Heck, no! As I mentioned, it’s a pretty new science. We know a few things, and are learning more each day. But getting sampled is a good starting point to understand what’s going on in your gut. And it helps science!
2. Consume some fermented foods/beverages daily.
Fermented foods are nutrient rich, containing vitamins, digestive enzymes, and probiotics. Adding probiotics to your diet can help repopulate your gut after times when it’s been compromised (e.g. after taking antibiotics or following a surgery).
Probiotics lower psychological distress and depression, decrease anger and hostility, lessen anxiety, and improve problem-solving. Eating fermented foods increases the diversity of good microbes in your gut (see #1).
Ahem, and we offer over 100 ways to craft your own probiotic-rich foods at home!
How much should you eat? Well, a little goes a long way. I recommend a small serving of fermented veggies (1/4 to 1/2 cup) before or with every other meal. If you like kombucha, about 16 ounces (500 ml) per day is quite enough! It is a tonic beverage, full of enzymes, probiotics, and organic acids, and should be treated as such.
3. Meditate daily.
A wise person once said, “We spend the first half of our lives building up our ego, and the second half breaking it down.” In my experience, meditation is the ego-slayer that almost every spiritual tradition acknowledges in some form or another. The practice of sitting quietly to connect with our deeper selves is an age old and effective path towards inner peace.
Is there a direct link between meditation and gut health? Well, we have recently discovered a bi-directional link between our brain and our gut via the vagus nerve.
Most of the serotonin (a feel-good chemical our bodies produce) is created in the gut. So it’s no exaggeration to say that a happy gut leads to a happy mood! There have also been studies showing that consuming certain strains of probiotics, known as psychobiotics, can lower psychological distress. These are “bottom-up” approaches (gut→brain), and perhaps a good start to our understanding. But meditation addresses our stress from the top-down (brain→gut), so to speak.
There are scant few studies I’ve found which directly measure the impact of meditation on our gut microbiome. Yet it is my own personal experience that reducing stress via meditation positively affects my overall health, which would necessarily include my gut microbiome.
There are loads of resources available to help you form a meditation practice. I would suggest starting simply.
How to Meditate
- Find a comfortable upright seated position. Could be in a straight backed chair, or cross-legged on the floor or on a couple of folded blankets. Do whatever your body is ready for– it’s important to feel comfortable. Your spine needs to be perpendicular to the earth. In this position, you literally become a connection between heaven and earth. Also, in this position, you won’t fall asleep.
- Try to meditate first thing in the morning, before life’s activities begin distracting you.
- Focus on your breath at first. Inhale and exhale slowly and deeply. This signals to your nervous system that all is well, and your physiological processes will follow suit.
- Your brain/ego will likely continue its monkey-mind chatter. Rather than try to push away or judge the thoughts, simply observe them, and don’t dwell, but let them go. One technique that works for me is to visualize placing each thought on a leaf, and setting the leaf into a stream to let it flow away.
- Sit as long as you can, gradually increasing to as much time as your schedule allows. Even ten minutes a day is a good start. Go easy on yourself. Meditation takes a lifetime (or more) to master!
4. Eliminate so-called “vegetable” oils from your diet altogether.
These so called “vegetable” oils (they’re more accurately seed oils) are made from plant seeds: sunflower, safflower, corn, canola (made from rapeseed, aka yu choy in Chinese, a plant in the cabbage family). They are all highly processed, being exposed to high heat, then they are filtered and deodorized to remove nasty byproducts. But most importantly, they are loaded with polyunsaturated fatty acids (fats or PUFA), specifically, lineolic and arachidonic acids, aka the “omega-6” fats. It is acknowledged that Western diets include far too much omega-6.
This is an especially inflammatory (pun intended) topic to investigate, because much of the research still clings to the now disproven hypothesis that saturated fats cause heart disease. So rather than advising us to simply reduce the overall amount of omega 6 in our diets, they encourage us to increase the omega-3 content in our diet to true up the ratio! It is true that the ratio of omega-3 to omega-6 is important, but to me that feels like a band-aid solution. Some studies show that increasing the overall omega-6 and omega-3 amounts has negative effects on our health, too. Too much omega-6 causes chronic inflammatory diseases such as nonalcoholic fatty liver disease (NAFLD), cardiovascular disease, obesity, inflammatory bowel disease (IBD), rheumatoid arthritis, and Alzheimer’s disease (AD).
It is not well understood or even known whether too much omega-6 has a direct impact on our gut bacteria. There have been a few studies that show that certain gut microbes can convert omega-6 into another nutrient, conjugated linoleic acid (CLA), but those studies admit that we don’t understand why. So there’s a gap in our understanding of causality of the direct effects of too much dietary omega-6, the effects are still clear.
So, how to eliminate this scourge of the Western society from your diet? Start reading labels and/or stop eating processed foods altogether! You’ll be shocked at how many processed foods contain one of these insidious fats. Almost all fried foods and snacks, cookies, crackers, bread (yep, even good ol’ bread, which should have flour, water, yeast and salt has been adulterated).
Switch to heart-healthy saturated fats from actual vegetables and fruits like avocado, olive, and coconut, or to animal fats from properly pasture raised animals.
5. Reduce/eliminate refined sugars from your diet.
There’s so much to say about sugar and its effect on humans. The typical Western diet contains too many refined simple sugars (sucrose, but also glucose and fructose). In my research, I found it difficult to find a study that isolates high sugar (versus high fat and high sugar) as a specific culprit, but it seems that there is agreement that too much sugar feeds the “wrong” gut bacteria like Clostridium dificile and C. perfringens, and in fact can affect the gut microbiota within one day. Having the wrong kinds of bacteria dominate in your gut is considered dysbiosis, although we are still in the infancy of what that means.
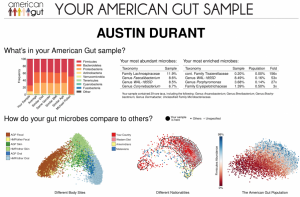
Research projects such as the American Gut Project seek to map out the contents of people’s gut microbiomes. By collecting thousands or even millions of samples, they are charting the composition and relative abundance of each species. Here are the results from my personal sample.
More complex carbohydrates (fiber, starches) are favored by the “good” bacteria. In fact, certain fibers are considered prebiotics because they specifically feed strains of good bacteria (but our own tissues cannot directly metabolize them).
Now, I have quite a sweet tooth myself, so I’m no sugar-free angel! A lot of recipes on this here blog are sweet! However, I try to make reasonable substitutions wherever possible, such as using honey instead of sugar when making items like ice cream kefir or sourdough granola. I tend to follow the “80/20” rule, making healthy choices at least 80% of the time, indulging about 20%. Find a ratio that works for you!
Author and founder of Fermenters Club. I’ve been fermenting food for 14 years.
In 2024, I published my first book, Fearless Fermenting.
When not stuffing things into jars, I enjoy permaculture gardening, cooking, yoga, writing, and studying cosmology and esoteric traditions.